For decades, diabetes meant lifelong insulin injections and constant monitoring. A recent stem-cell experiment in Shanghai has begun reshaping that expectation. One patient with long-standing Type 2 diabetes reportedly stopped insulin after receiving lab-grown insulin-producing cells derived from his own stem cells — a development that signals real biological repair rather than temporary control.
🧬 How Scientists Rebuilt Insulin Production
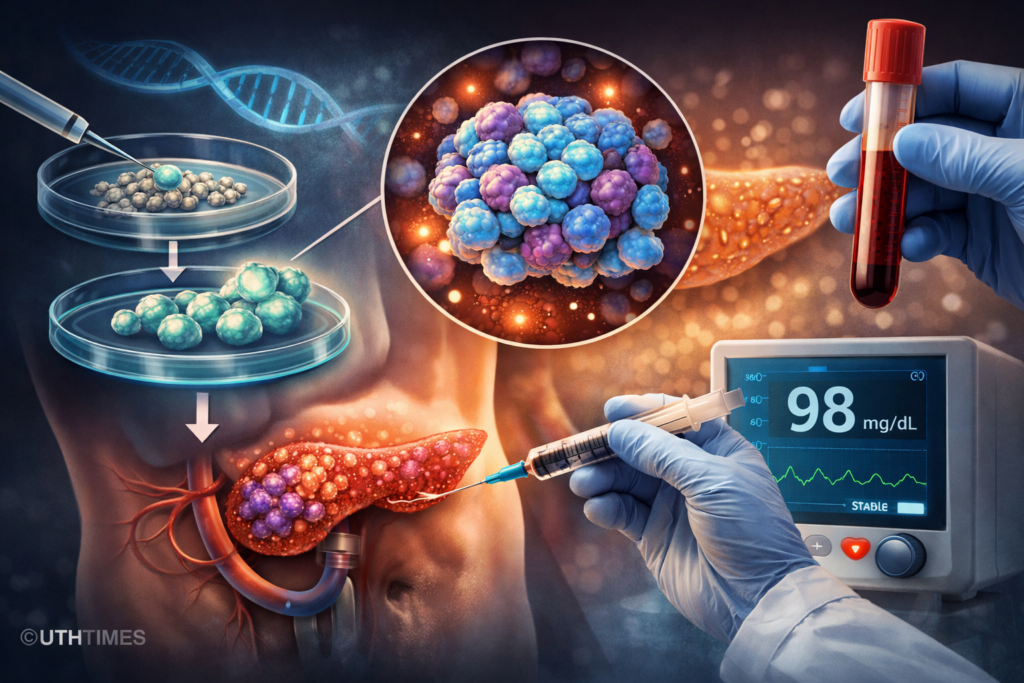
Researchers developed insulin-secreting beta-like cells from the patient’s own stem cells and transplanted them into his body. Instead of controlling blood sugar externally, this therapy aims to restore the pancreas’s natural function.
Key elements of the procedure:
🔬 Patient-Derived Stem Cells
Scientists reprogrammed the patient’s cells into pluripotent stem cells, minimizing immune rejection risks and avoiding donor dependence.
🧪 Engineered Beta Cells
The stem cells were converted into functional insulin-producing cells designed to respond dynamically to glucose levels.
💉 Precision Transplantation
The regenerated cells were implanted into a region with strong blood supply so they could detect glucose and release insulin naturally.
📊 Medical Monitoring
Detailed blood tests and imaging showed stable glucose control without insulin injections — the strongest evidence that the cells were functioning like a biological pancreas.
This marks one of the clearest human demonstrations that beta-cell replacement therapy can move beyond laboratory experiments.
🌍 Why This Case Matters Worldwide

The Shanghai case represents a shift from managing diabetes to potentially repairing the underlying damage.
Its importance extends far beyond one patient:
🌍 Human Proof of Regeneration
Beta-cell therapies have shown promise in animals, but real human evidence has been limited.
💉 Reducing Lifetime Insulin Dependence
If replicated, future patients may rely less on daily injections and monitoring.
🧠 Personalized Regenerative Medicine
Using a patient’s own cells suggests safer and more individualized therapies.
🏥 A Blueprint for Future Treatments
The procedure creates a clinical pathway for larger trials and improved methods.
For millions living with diabetes, the idea that insulin-producing cells can be rebuilt is a major scientific shift.
⚠️ The Limits Scientists Emphasize

Despite the excitement, researchers stress that this is an early-stage clinical observation.
Key uncertainties remain:
🔍 Durability of the Cells
Scientists must determine whether the regenerated beta cells will function for many years.
🧬 Cost and Complexity
Personalized stem-cell therapy requires advanced laboratories and specialized expertise.
📈 Need for Larger Studies
A single successful patient cannot define a universal treatment.
⚕️ Different Diabetes Types
It is still unclear how well this method could work for Type 1 diabetes.
Scientific validation will require multi-patient clinical trials and long-term monitoring.
🔮 A Glimpse of Diabetes Treatment’s Future

The Shanghai study offers something rare in diabetes research — visible biological recovery instead of disease management. If future trials confirm these findings, diabetes care may shift from lifelong insulin therapy toward regenerative solutions.
For now, the result stands as a powerful signal that rebuilding insulin production in humans may no longer be a distant idea — but an emerging medical reality.
